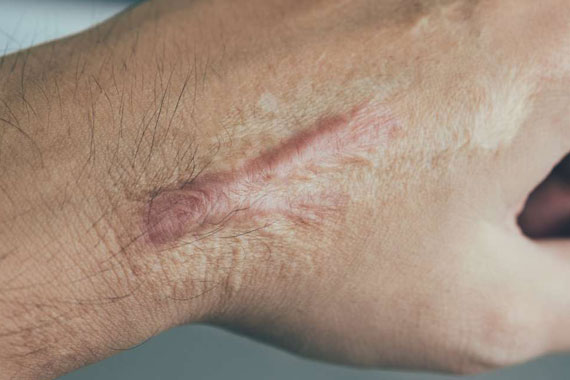
Not to do list: when suffering with keloids
Keloid in dark population is more than 10%. Though it is so common, no uniformly effective treatment is available. Any unwarranted injury has a potential to develop a keloid. So avoidance of injury is the best strategy. Try to avoid un necessary surgery. Following procedure have high risk of keloid formation in keloid prone individuals
Tattoo
Reaction to Tattoo ink is common. Tattoo injury itself or tattoo ink reaction can trigger new keloid in predisposed individuals. If you have even a small keloid, refrain from this activity.
Laser tattoo removal
Laser tattoo removal in keloid patient has fairly high potential of developing new keloid. So don’t opt for tattoo removal unless it is really necessary. Choose an experienced dermatologist who has expertise of avoiding keloid or treating keloids.
Deep chemical peels or laser surgeries
Deep chemical peels are NOT safe in dark skin. They cause burn which can lead to keloids in predisposed individuals. Same is about ablative lasers like CO2 or Er YAG or MNRF.
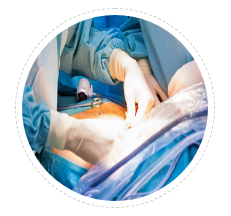
Surgeries
Slowly healed wound of surgery, inflammatory reaction to stitch thread can initiate keloid. Your surgeon need to have expertise of anticipating and treating keloids. Or else involve your keloid treating doctor in surgical plan or see him immediately after suture removal to plan keloid prevention.
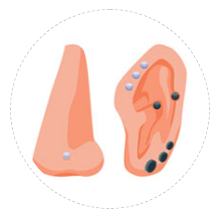
Nose ear or body piercing
In prone individuals body piercing has very high chance of recurrence of keloid so it is better avoided.