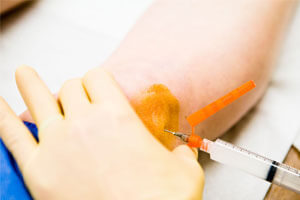
Keloid: know the basics.
Genetics: what is keloid tendency? Is keloid genetic disease ?
Keloid has very much diverse and varied presentations. It may present as a single or multiple, discrete or confluent , thin linear lesions or large giant nodular patches. This variety of presentations hints at complex and multi-gene inheritance. Those having a mutation (change) in a single gene may have single or less severe keloid while those with multiple faulty genes may show more aggressive pattern of keloids. Specific genes are reported in Chinese and Taiwan population but larger studies are required to know which genes are at fault in each population. Such studies in India are missing and skincity is planning to take up one genetic study on Indian pattern of inheritance.
Genetically predisposed individuals develop Keloids after injury to the skin that acts as a trigger. This triggering injury could be anything from minor inflammatory skin condition, acne, chicken pox, vaccination; to body piercing, surgical wounds, burns, etc. Though not all keloid prone individuals or all those with family history will develop keloid, while in the same keloid patient, not all injuries will evolve into keloids.
How many members in family have developed keloid is another predictive factor for severity of keloid. How many siblings, father, mother or both? How many generations?


Race and ethnic distribution
Dark-skinned individuals of African, Asian, and Hispanic descent have higher rates of keloid development compared to Caucasians. The incidence in these darker-pigmented populations ranges from 4.5% to 16%. The incidence is notably higher during pregnancy and puberty. A positive family history increases the risk for the development of keloids although no specific gene has been identified. The chance of getting keloid, its severity and chance of it running in family increases with skin colour. Incidence of keloid is zero in albinos while least in white skinned Caucasians while moderate in brown coloured Indian and worst in dark coloured Africans. This clearly signifies the importance of melanin or skin colour.
In India also there is wide variation in skin shade across north to south of the country. It would be interesting to compare epidemiology of various ethnic groups in India. SkinCity has initiated such a research on epidemiology.
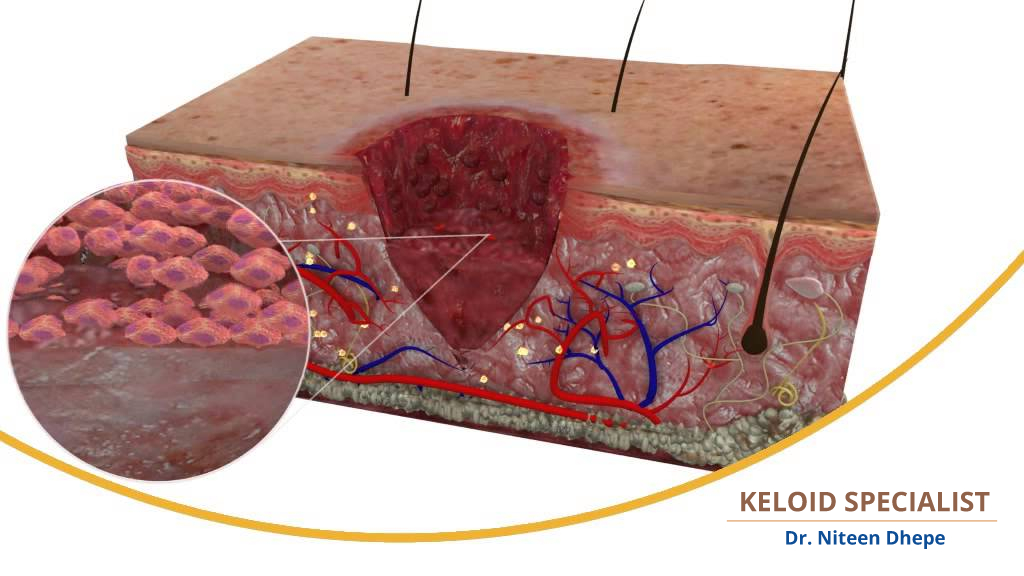
Pathophysiology: what's going wrong in keloid formation?
Keloids are a result of aberrant wound healing process. What is going wrong in wound healing here? Standard wound healing consists of three phases: (1) inflammatory (swelling), (2) fibroblastic (collagen formation), and (3) maturation (collagen remodelling) . In keloids, the fibroblastic phase continues, unchecked. Keloidal fibroblasts work harder, persist for longer, and have lower rates of apoptosis (don’t die early!) compared to ‘normal’ wound healing resulting in an overproduction of collagen. Collagen synthesis in keloids is 20 times greater than that of healthy skin and three times greater than a hypertrophic scar.

Keloid Pathology
Keloid: a disease of darker skin type
Keloid is basically a disease of skin of color. Very few in Caucasians are affected by keloids, while most severely affected community is African Americans. In between lies a variety of skin shade called Asian skin. Asian skin is again classified as yellow in far Asian like china and japan while brown in Indian subcontinent. Even in India a variety of ethnic subgroups show wide variations of skin color from light brown north Indians to dark brown south Indians. The prevalence of keloid in darker population ranges from 6 to 15% it would be interesting to observe differences between these subgroups.
Though number of people suffering from keloid may be more than ten crores, As this is a disease of dark skin and poor world, it has not attracted the attention or funding of scientific community. So indigenous research by local stake holders will be very much valuable. SkinCity has launched various research projects for keloids.
Trigger factors: what makes keloid worse?
Ok. Keloid occurs in genetically predisposed individuals and when a deep non healing or slowly healing wound occurs. But why only at certain age? Why only at certain places? Why some keloids on some body parts grow larger than other body parts? It is highly unpredictable though some patterns are observed.
What injury? previous skin trauma or inflammation. Lesions may develop as early as 1 to 3 months or as late as one year after injury. Spontaneous lesions are reported. Those may be due to very minor injury was not recalled or keloid might have developedafter months or even years of injury.
what are aggrevating factors
Traction and tension?
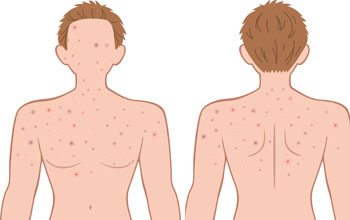
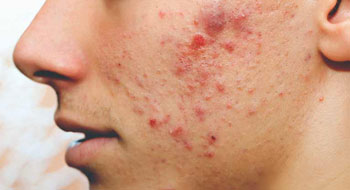
Acne or pimple
Surgery makes keloid worse
Keloid creams and steroid injections